What is a Herniated Disc?
On This Page
A herniated disc, also called a slipped disc or prolapsed disc, is when a soft cushion of tissue between the bones in your spine bulges outwards or when the disc moves from its natural position. It’s painful if it presses on spinal nerves.
Herniated discs affect roughly 1% to 3% of adults annually. It is most common in people aged 30 to 50 and men are affected twice as often as women.
Most cases resolve naturally within 6-12 weeks. However, 10% of patients with persistent symptoms require surgical intervention.[1]
Key Facts
-
Also known as
- Slipped disc, prolapsed disc
-
Prevalence
- Affects 1-3% of adults annually; most common at ages 30-50 and in men
-
Symptoms
- Chronic lower back pain, sciatica, numbness or weakness in the legs
-
Diagnosis
- Confirmed by lumbar MRI scan
-
Outlook
- Around 90% of patients experience relief within 6-12 weeks, but 10% of cases require surgical intervention
Herniated Disc Symptoms
Significantly herniated discs in the lumbar spine typically cause:
- Chronic sciatica – pain in the buttocks, hips or legs when the disc presses on the sciatic nerve
- Acute band-like lumbar pain increased by exertion, driving, static sitting and standing
- Episodes of spinal blocking and inability to move
- Severe lower back pain
- Significantly impaired mobility
- Problems bending or straightening your back
- Muscle weakness
- Numbness or tingling in the leg, foot or toes
What Causes a Herniated Disc?
Herniated discs are usually the result of gradual disc degeneration. Over time, the intervertebral discs lose water content and become less flexible, and the tough outer layer (the annulus fibrosus) weakens. Eventually, the soft cushion of tissue inside the disc (the nucleus pulposus) can push through a tear in the outer layer, causing the disc to bulge or move from its natural position. When this process of degeneration causes ongoing symptoms which steadily deteriorate over time, it is known as degenerative disc disease.
Several factors increase the likelihood of disc degeneration and herniation:
- Ageing, as discs naturally lose hydration and elasticity over time
- Genetics – some people inherit a predisposition to disc degeneration
- Occupations or habits involving heavy lifting, prolonged sitting, or driving for long periods of time
- Smoking, which reduces blood supply to the discs and accelerates degeneration
- Being inactive or overweight
While disc degeneration is the underlying cause, a specific herniation is often triggered by a particular movement, such as lifting heavy objects the wrong way, twisting awkwardly, or exercising too hard.
Why Are You in Pain?
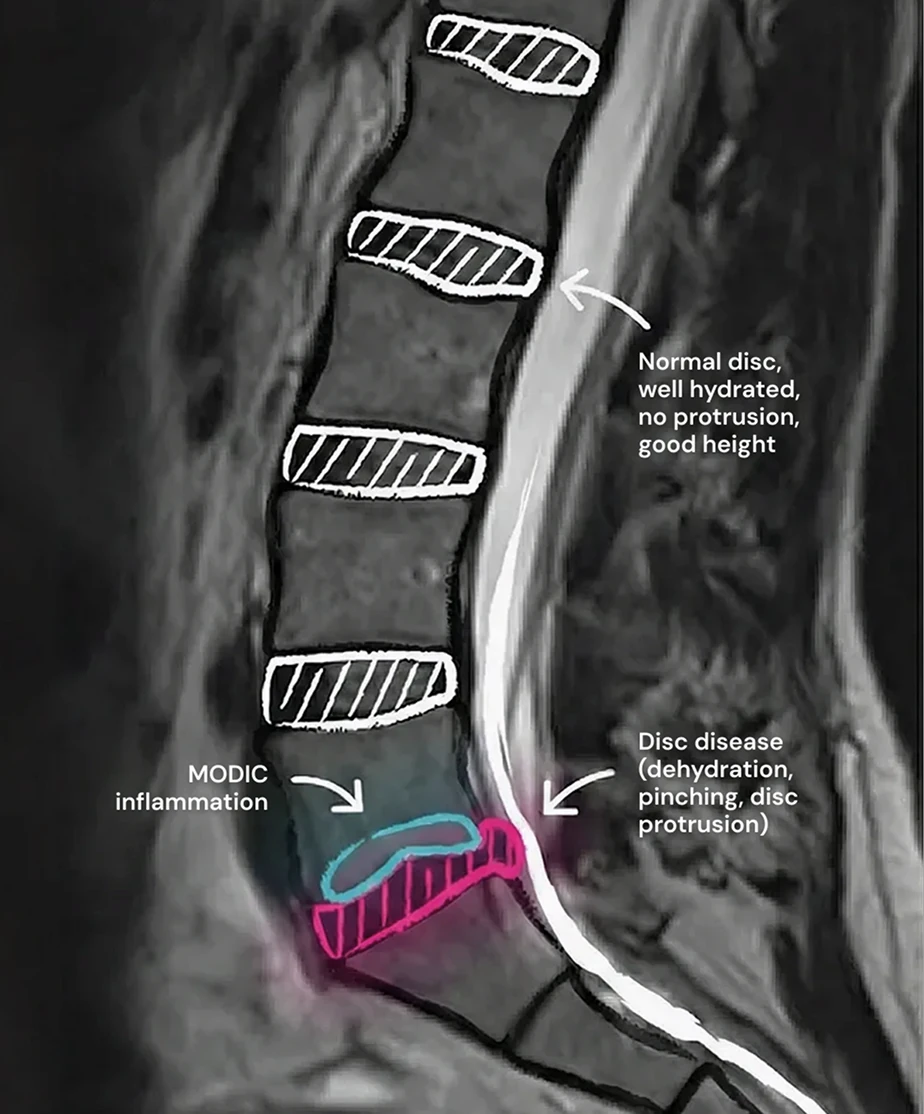
In cases of significant herniation, the disc (or disc fragments) can compress spinal nerves, resulting in chronic sciatica in one or both legs and the gluteal region. The disc itself may also become dehydrated, bulging (protrusion), and sometimes inflamed, causing pain without direct nerve compression.
Do They Heal on Their Own?
Mild symptoms often resolve themselves. However, once repeat symptoms become severe and more frequent, they normally steadily deteriorate until surgical intervention is required.
What Treatments are Available?
Treatments for herniated discs vary depending on the severity of the symptoms. For mild cases, painkillers, physiotherapy and walking will help to resolve symptoms naturally. If the frequency and severity of symptoms increase, other options include steroid injections, and surgical intervention such as discectomy, spinal fusion, and total lumbar disc replacement.
How Does SpinePro Treat Herniated Discs?
SpinePro, in conjunction with CCV Montpellier, offers Prodisc® L total lumbar disc replacement, a minimally invasive surgical procedure which fully restores spinal mobility and permanently relieves symptoms in a single procedure by safely replacing the degenerated natural disc with an artificial disc.
If you have a lumbar MRI scan less than 6 months old, contact SpinePro for your free surgical assessment to see if you are a candidate for total lumbar disc replacement.
Frequently Asked Questions
What is the difference between a slipped disc and a herniated disc?
There is no difference. Slipped disc is simply the common name for a herniated disc. Doctors may also use the term prolapsed disc. All three refer to the same condition.
What is the difference between a herniated disc and a bulging disc?
A bulging disc extends outward but remains intact. A herniated disc has a tear in its outer layer, allowing the inner material to push through. Herniated discs are more likely to compress nearby nerves and cause symptoms like sciatica.
How do you know if you have a herniated disc?
Common signs include severe lower back pain, chronic sciatica (pain radiating down one or both legs), numbness or tingling in the legs or feet, and muscle weakness. However, a lumbar MRI scan is needed to confirm the diagnosis.
Can a herniated disc cause permanent nerve damage?
In most cases, no. The majority of herniated discs heal without lasting damage. However, prolonged or severe nerve compression can cause persistent numbness, weakness, or chronic pain.
Which discs are most commonly affected?
The vast majority of lumbar disc herniations occur at the L4-L5 or L5-S1 levels – the two lowest discs in the spine. These discs bear the most weight and experience the greatest mechanical stress, making them more susceptible to degeneration and herniation.
Is a herniated disc the same as degenerative disc disease?
No. Degenerative disc disease (DDD) is the gradual breakdown of the spinal discs over time. A herniated disc is often a consequence of this degeneration, when a weakened disc finally tears, bulges, or moves from its natural position. You can have DDD without a herniation, but most herniations occur in discs that have already degenerated.
References
- Lumbar Disc Herniation – StatPearls