What Is Degenerative Disc Disease?
On This Page
- What Is Degenerative Disc Disease?
- What Causes Degenerative Disc Disease?
- How Common is Degenerative Disc Disease?
- Common Symptoms of Degenerative Disc Disease
- Treating Degenerative Disc Disease
- Degenerative Disc Disease and Related Conditions
- How Does SpinePro Treat Degenerative Disc Disease?
- Frequently Asked Questions
Degenerative disc disease (DDD) is a condition where one or more intervertebral discs deteriorate, causing pain (usually in the lower back or neck) with or without sciatica. The condition is also referred to as disc degeneration or intervertebral disc degeneration. When affecting the lower back specifically, it may be called lumbar disc disease; in the neck, cervical disc disease.
There is no universal medical definition. Some doctors apply the term to any visible disc changes; others reserve it for cases causing significant symptoms. Here, we use it to mean lumbar disc deterioration that results in persistent symptoms and chronic pain.
Key Facts
-
Cause
- Caused by ageing, genetic factors, or accidental damage
-
Effect
- Dehydration and hardening of discs, which may move from their natural position (herniate) and compress nearby spinal nerves or cause inflammation between vertebrae
-
Location
- Most common in the lumbar spine (lower back) due to the weight it bears
-
Diagnosis
- Confirmed by lumbar MRI and CT scans
-
Treatment
- Ranges from medication combined with physical therapies to surgical interventions such as total lumbar disc replacement
What Causes Degenerative Disc Disease?
Intervertebral discs wear out over time and dehydrate, causing the gel-like nucleus pulposus to escape. This in turn allows the disc to move from its natural position, often causing inflammation or compressing spinal nerves.
When this degeneration is sufficient to cause symptoms, it’s termed degenerative disc disease. Contributory factors include natural ageing, genetics, spinal injuries, smoking, and occupations involving heavy lifting or prolonged sitting.
What Are Intervertebral Discs?
Intervertebral discs are the shock-absorbing structures between vertebrae. Each has a tough exterior and a soft gel-like centre (the nucleus pulposus). The lumbar spine’s five discs support most of the body’s weight, making them especially susceptible to wear.
What Happens When Discs Degenerate?
As discs degenerate, they dehydrate and compress under the weight of the vertebrae above and below. The outer layer may develop tears, allowing the nucleus pulposus to leak out and the disc casing to bulge. Disc material pressing on the lower spinal nerve roots causes sciatica, a pain that follows the path of the sciatic nerve down the leg.
How Common is Degenerative Disc Disease?
Almost everyone develops some disc degeneration with age. Most never notice. The term degenerative disc disease is typically applied when degeneration causes ongoing symptoms, which affects a minority.
In our experience, up to 10% of patients experience symptoms which get that progressively worsen and require surgical intervention, such as total lumbar disc replacement.
Common Symptoms of Degenerative Disc Disease
The main symptoms of lumbar degenerative disc disease are severe lower back pain and chronic sciatica. Symptoms often fluctuate, with flare-ups triggered by activity or sustained postures, and periods of relative relief. Over time, a minority of patients experience an increased frequency of episodes with more severe symptoms that cannot be managed by medication and physical therapies.
For this group, symptoms have a detrimental effect on their quality of life, making routine daily activities, sleeping, and working difficult, if not unbearable.
Treating Degenerative Disc Disease
Treatment begins with conservative measures: including pain medication, physiotherapy, and activity modification, typically trialled for several months. Surgery is considered when these approaches are ineffective in adequately controlling symptoms. Options include steroid injections (which provide temporary relief from inflammation), discectomy (which relieves nerve compression and may provide temporary relief of symptoms), spinal fusion, and Prodisc® L total lumbar disc replacement.
Degenerative Disc Disease and Related Conditions
Several terms overlap with degenerative disc disease, which can cause confusion.
A herniated disc occurs when the gel-like nucleus pulposus pushes through a tear in the disc’s outer layer, deforming the disc and allowing it to move from its natural position. This can cause symptoms such as severe lower back pain and sciatica. Slipped disc means the same thing.
Herniation is often a consequence of disc degeneration, but not everyone with degenerative disc disease develops a herniation.
Sciatica refers to pain radiating from the lower back into the buttock and leg, following the path of the sciatic nerve. It is a symptom rather than a diagnosis, and disc herniation is one of its most common causes.
How Does SpinePro Treat Degenerative Disc Disease?
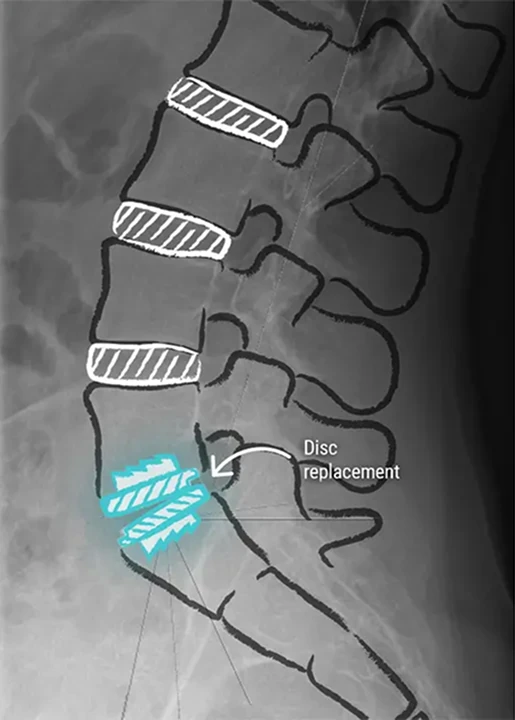
SpinePro offers Prodisc® L total lumbar disc replacement, a minimally invasive surgical procedure designed to restore spinal mobility and provide lasting symptom relief by replacing the degenerated natural disc with an artificial disc.
Frequently Asked Questions
Is degenerative disc disease hereditary?
Genetics appear to influence susceptibility to disc degeneration. If close relatives have the condition, your risk may be elevated. However, heredity is one factor among several, including occupation, injury history, and lifestyle.
Is degenerative disc disease the same as a herniated disc?
No. Degenerative disc disease describes the deterioration of intervertebral discs over time. A herniated disc is one possible result: the weakened outer layer fails and the nucleus pulposus pushes through. You can have degeneration without herniation, but most herniations occur in significantly degenerated discs.
Can degenerative disc disease be cured or reversed?
Disc degeneration cannot be reversed. The symptoms, however, can be treated effectively. Many people manage with physical therapies and medication. When conservative treatment is insufficient, surgery such as total lumbar disc replacement can provide permanent relief by replacing the degenerated disc with an artificial disc.
Why is it called degenerative disc disease?
The name is imprecise. Degenerative means gradual breakdown. Disease in medical terminology doesn’t always imply an illness that spreads. The term describes a process rather than a progressive disease, which is why some doctors prefer simply disc degeneration.
Will I need surgery for degenerative disc disease?
Most people don’t. Surgery is typically considered only when conservative treatments can no longer control worsening symptoms.
Without paralysis or severe neurological problems, surgery is an option rather than a necessity. Following your surgical assessment, your SpinePro surgeon can discuss whether surgery is appropriate and whether you are a suitable candidate.